When someone spends hours every day playing video games-not just for fun, but because they can’t stop-it’s not always just about entertainment. For many, it’s a way to escape. And when that escape turns into a pattern that interferes with work, relationships, or sleep, it may be Internet Gaming Disorder (IGD). But here’s what most people don’t realize: IGD doesn’t usually show up alone. It often travels with another invisible weight-depression.
What’s the real link between depression and gaming disorder?
Studies from 2023 to 2025 show that between 38% and 52% of people diagnosed with Internet Gaming Disorder also meet the clinical criteria for major depressive disorder. That’s more than one in two. These numbers come from pooled data across 12 large-scale studies in North America, Europe, and East Asia, involving over 15,000 participants aged 13 to 40.
It’s not that gaming causes depression, and it’s not that depression causes gaming. It’s a loop. People with depression often feel numb, isolated, or overwhelmed by real-life stress. Video games offer a world where they can control outcomes, earn rewards, and feel connected-even if it’s virtual. The more they play, the more their real-world responsibilities slip. The worse their real life gets, the more they retreat. And the cycle tightens.
How do researchers measure this connection?
Researchers use two main tools: the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) criteria for IGD, and the Patient Health Questionnaire-9 (PHQ-9) for depression. IGD is diagnosed when someone has at least five of nine symptoms over 12 months-like preoccupation with gaming, withdrawal symptoms when not playing, lying about usage, and continuing despite negative consequences.
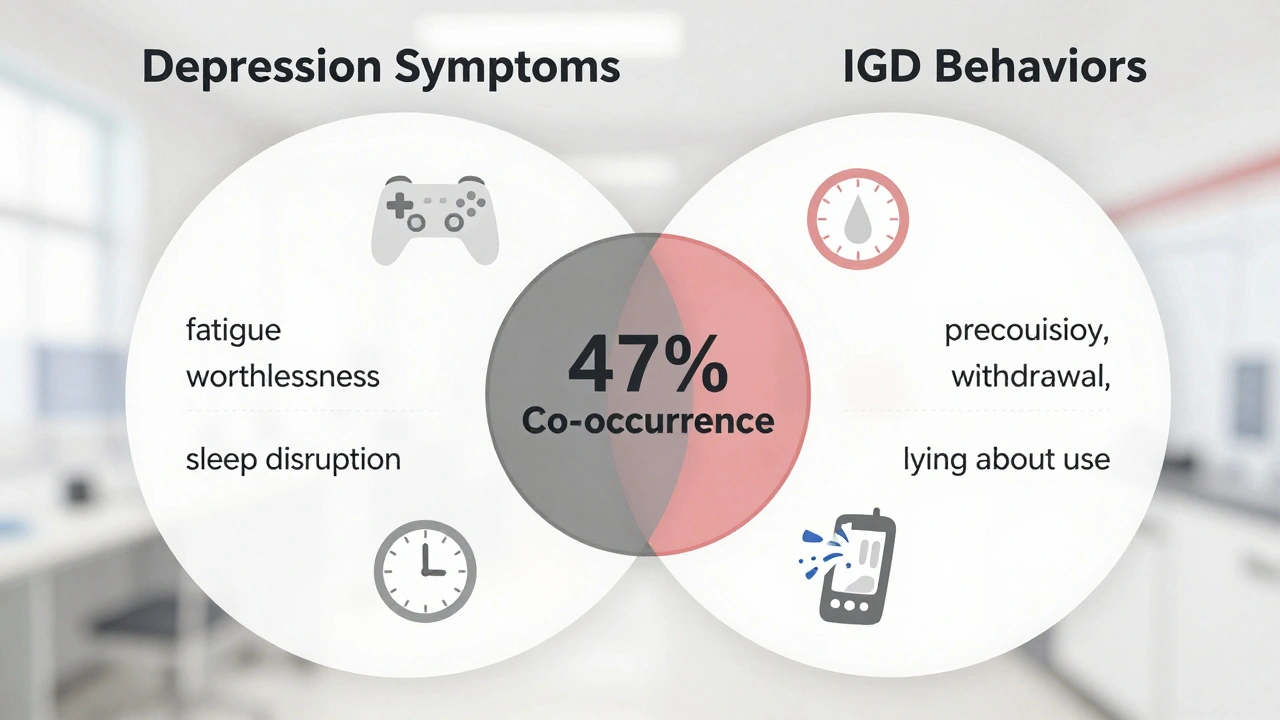
Depression is measured by scoring 10 or higher on the PHQ-9, which tracks symptoms like low mood, fatigue, sleep issues, and feelings of worthlessness. In a 2024 meta-analysis of clinical samples, 47% of those who scored high on IGD also scored above the clinical threshold for depression. The reverse was true too: people with moderate to severe depression were 3.2 times more likely to develop IGD than those without depression.
Who’s most at risk?
The highest overlap isn’t in teens-it’s in young adults aged 18 to 25. This group faces unique pressures: transitioning out of school, unstable jobs, social isolation, and financial stress. For them, online games aren’t just a hobby. They’re a coping mechanism. A 2025 study tracking 3,000 university students found that those who played more than 30 hours a week were 4.1 times more likely to have both IGD and depression than those who played under 10 hours.
Gender also plays a role. While men are more likely to be diagnosed with IGD, women with depression are more likely to develop gaming dependence as a way to manage emotional pain. In one cohort, 58% of women with clinical depression who developed IGD reported using games to numb anxiety, while 63% of men cited social connection as their main driver.
What does this look like in real life?
Take Maria, 22, from Berlin. She dropped out of college after her second semester. She stopped answering texts. She slept during the day and played a massively multiplayer game from midnight to 7 a.m. every night. Her therapist found she had been diagnosed with depression six months earlier but hadn’t sought treatment. When asked why she didn’t stop gaming, she said, “It’s the only place I feel like I’m good at something.”
Or James, 20, in Seoul. He played 14 hours a day, every day. His parents took away his laptop. He bought a second one with his savings. He skipped meals. He lost 18 pounds in three months. His doctor found he’d been self-medicating depression with gaming for over two years. He wasn’t addicted to the game-he was addicted to the feeling of control it gave him.
Why do traditional treatments often fail?
Most mental health programs treat depression and gaming separately. But that’s like trying to fix a leaky roof while ignoring the storm outside. When someone with IGD and depression is told to “just play less,” without addressing the underlying sadness, they often relapse. Studies show that treatments combining cognitive behavioral therapy (CBT) for depression with behavioral interventions for gaming-like setting structured play limits and rebuilding real-world routines-have a 68% success rate over six months. Treatments that only target gaming have a failure rate over 70%.
One key intervention is called “replacement behavior therapy.” Instead of just cutting gaming time, therapists help patients build small, rewarding activities in real life: walking in the park, cooking a meal, calling a friend. These activities trigger the same dopamine release as gaming, but without the consequences. Over time, the brain starts to associate real-world actions with pleasure-not just screens.

What about prevention?
Early signs matter. If a teenager starts skipping meals to game, avoids eye contact, or says things like “I only feel alive when I’m playing,” it’s not just teenage behavior. It’s a red flag. Schools in Japan and Sweden now screen students for both depression symptoms and gaming patterns in health classes. They don’t ban games. They teach balance. They ask: “What are you avoiding when you play?”
Parents can help too-not by confiscating devices, but by noticing changes. If your child used to talk about friends, school, or hobbies, and now only talks about game levels or rankings, that’s a signal. It’s not about how much they play. It’s about what they’re not doing anymore.
What’s next for treatment and research?
Researchers are now testing apps that track gaming patterns and mood in real time. One pilot app, used in 1,200 patients across Germany and Canada, sends alerts when someone plays more than 5 hours straight and reports low mood. It then suggests a 10-minute breathing exercise or connects them to a peer support group. Early results show a 40% reduction in daily gaming time and a 35% drop in depression scores over eight weeks.
Another promising area is neuroimaging. Brain scans show that people with both IGD and depression have reduced activity in the prefrontal cortex-the part responsible for decision-making and impulse control. This isn’t weakness. It’s biology. And that means treatment needs to be medical, not moral.
Bottom line: It’s not about the game
Depression and Internet Gaming Disorder are two sides of the same coin. One doesn’t cause the other-but they feed each other. And treating one without the other rarely works. The goal isn’t to stop gaming. It’s to help people find meaning, connection, and control outside of screens. When that happens, the games lose their power.
Is Internet Gaming Disorder officially recognized as a mental illness?
Yes. The World Health Organization included Internet Gaming Disorder (IGD) in the 11th Revision of the International Classification of Diseases (ICD-11) in 2018. It’s classified as a behavioral addiction. To be diagnosed, symptoms must be severe enough to cause significant impairment in personal, family, social, educational, or occupational functioning for at least 12 months.
Can someone have IGD without being depressed?
Yes. While depression is the most common co-occurring condition, not everyone with IGD is depressed. Some people develop gaming dependence due to social anxiety, ADHD, or trauma. But even in those cases, depression often develops over time as isolation and neglect of basic needs take a toll. Screening for depression is still recommended in all IGD cases.
How many hours of gaming is too much?
There’s no universal number. A person playing 4 hours a day might be fine if they’re sleeping well, holding a job, and maintaining relationships. The red flags are when gaming replaces basic needs-like eating, hygiene, or social contact-or when someone feels anxious, irritable, or empty when not playing. It’s not about time. It’s about function.
Are certain types of games more likely to cause IGD?
Massively multiplayer online games (MMOs), battle royales, and loot-box based games show the highest rates of IGD. These games are designed with constant rewards, social pressure, and unpredictable outcomes-features that strongly activate the brain’s reward system. Single-player games with clear endings are less likely to trigger dependency, though they can still be problematic if used to escape emotional pain.
Can medication help with IGD and depression together?
Antidepressants like SSRIs (e.g., sertraline or escitalopram) can help reduce depressive symptoms, which may indirectly reduce gaming urges. But medication alone doesn’t change gaming behavior. The most effective approach combines medication with behavioral therapy. Studies show that patients on SSRIs who also received CBT for gaming had a 62% improvement rate compared to 28% with medication only.
